Kids are more susceptible to head injury than previously thought

Head knocks in childhood are by no means uncommon, yet they may have lasting negative effects. New research has found a link between concussion in childhood and adverse medical and social outcomes as an adult.
Researchers from the United Kingdom, United States and Sweden looked at data from the entire Swedish population born between 1973 and 1982 – some 1.1 million people – to analyse the effect of experiencing a traumatic brain injury in the first 25 years of life.
Compared to those who had sustained no injury, people who had experienced at least one traumatic brain injury in childhood – around 9% of those studied – were, as adults, more likely to die early or be treated for a psychiatric illness and receive a disability pension, and less likely to have completed secondary schooling.
At first glance, the findings seem unsurprising: common sense suggests, for example, that a child who has sustained severe brain damage in a car accident would encounter more educational obstacles than a child who hasn’t.
Accordingly, the study found that the more severe the brain injury, the worse the outcomes in adulthood (this was also the case for repeated brain injuries). But the research also found a significant link between concussion – the mildest and most common form of brain injury – and subsequent problems.
In the study, concussions comprised more than 75% of the childhood brain injuries recorded. The researchers found being exposed to a concussion, or mild brain injury, was associated with a 18%–52% increased risk of negative outcomes, including early death, low educational attainment, and being on welfare. The most marked increase in risk was found for psychiatric inpatient hospitalisation and the disability pension.
Traumatic brain injury and concussion – the same thing?
Traumatic brain injury occurs when the brain is damaged by external force such as a fall, car accident, assault or being struck by an object such as might occur during sport. It’s usually classified according to its severity, or based on the anatomy of the injury. Moderate to severe traumatic brain injury can result in irreversible structural damage to the brain, and in some cases death.
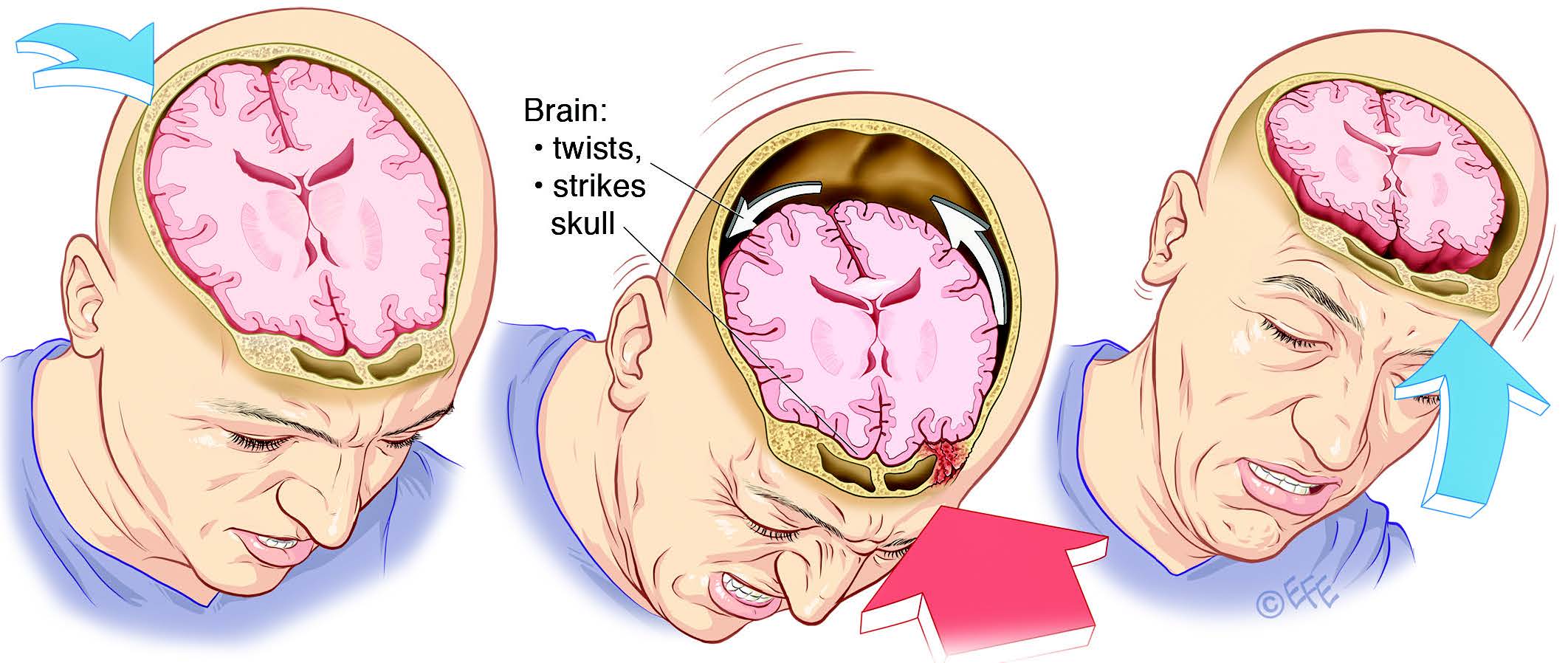
A concussion, on the mild end of the brain injury spectrum, results when force causes the brain to twist upon itself or strike the skull. Bruising and cell damage can occur, but any structural damage from the injury cannot be picked up by MRI or CT imaging, which can make diagnosis difficult. Using specialised imaging methods such as functional MRI (fMRI), however, changes in patterns of brain activity are apparent soon after a concussion.
Research shows even a seemingly innocuous knock that wouldn’t qualify as a concussion can trigger changes in brain physiology and affect the functioning of neurons. There is some evidence that repeated concussions could be associated with the development in later life of a neurodegenerative disease called chronic traumatic encephalopathy. More long-term research is needed to determine how permanent or reversible brain changes following a single concussion are.
The new study found an association between the age at first head injury and subsequent health and social outcomes. Children who were older, and particularly those who were older than 15, were substantially more likely to have problems in adulthood.
Although the study findings are yet to be replicated, the authors suggest heightened neuroplasticity – the ability of the brain to adapt and change its networks and behaviour – in younger years may be protective in the long term.
Protecting young brains
While there are still many unknowns when it comes to concussion, the latest findings point to the importance of minimising head trauma in childhood. Because children have weaker necks and torsos than adults, less force is needed to cause a brain injury. For toddlers and preschoolers, the study’s authors suggest improved parental supervision is key, as falls are the most common cause of traumatic brain injury for young children.
In older children, reducing the incidence of sports-related concussions may be trickier. Wearing hard helmets in sports generally reduces the risk of severe head injuries such as skull fractures and bleeding inside the skull, but is ineffective against the rotational forces – forces that cause the head to turn rapidly and the brain to twist on itself, as can occur with whiplash for example – that can cause concussion. There’s also no evidence that the soft headgear worn in some Australian football codes can protect against brain injury.
Many concussions occur without noticeable signs such as disorientation or slurred speech, and for that reason go undiagnosed. The danger of an unrecognised concussion on the sporting field – which predisposes a player to subsequent concussion – is that it increases the risk of lasting damage. The lack of awareness about the symptoms, treatment and management of concussion is an unrecognised public health problem.

The health benefits of sport are well established and should be supported. However, the nature of contact sports means that head knocks are sometimes unavoidable.
Given Australia’s strong sporting culture, the solution is not to change the fundamental rules of these sports or prevent children from playing them. Rather, by investing in research and improving awareness at the grassroots level, we can improve the diagnosis and management of concussive episodes in kids.
***
This article has also appeared on The Conversation.



