Depression and the brain
Key depression facts
- Depression involves an overemphasis of negative emotions and a decrease in the reward produced by pleasurable experiences.
- Chronic stress can be important in the development of depression.
- An inability to cope with stress causes changes in how the brain balances positive and negative information.
- Key structures include the prefrontal cortex, amygdala, nucleus accumbens, and hippocampus.
Stress as a trigger for depression
Although the onset of depressive episodes can typically be traced to high levels of stress, stress alone is not enough. All of us are exposed to stressors, admittedly of varying intensity and duration, but only some of us develop major depression. It’s really a failure to cope with stress that can trigger the descent into depression.
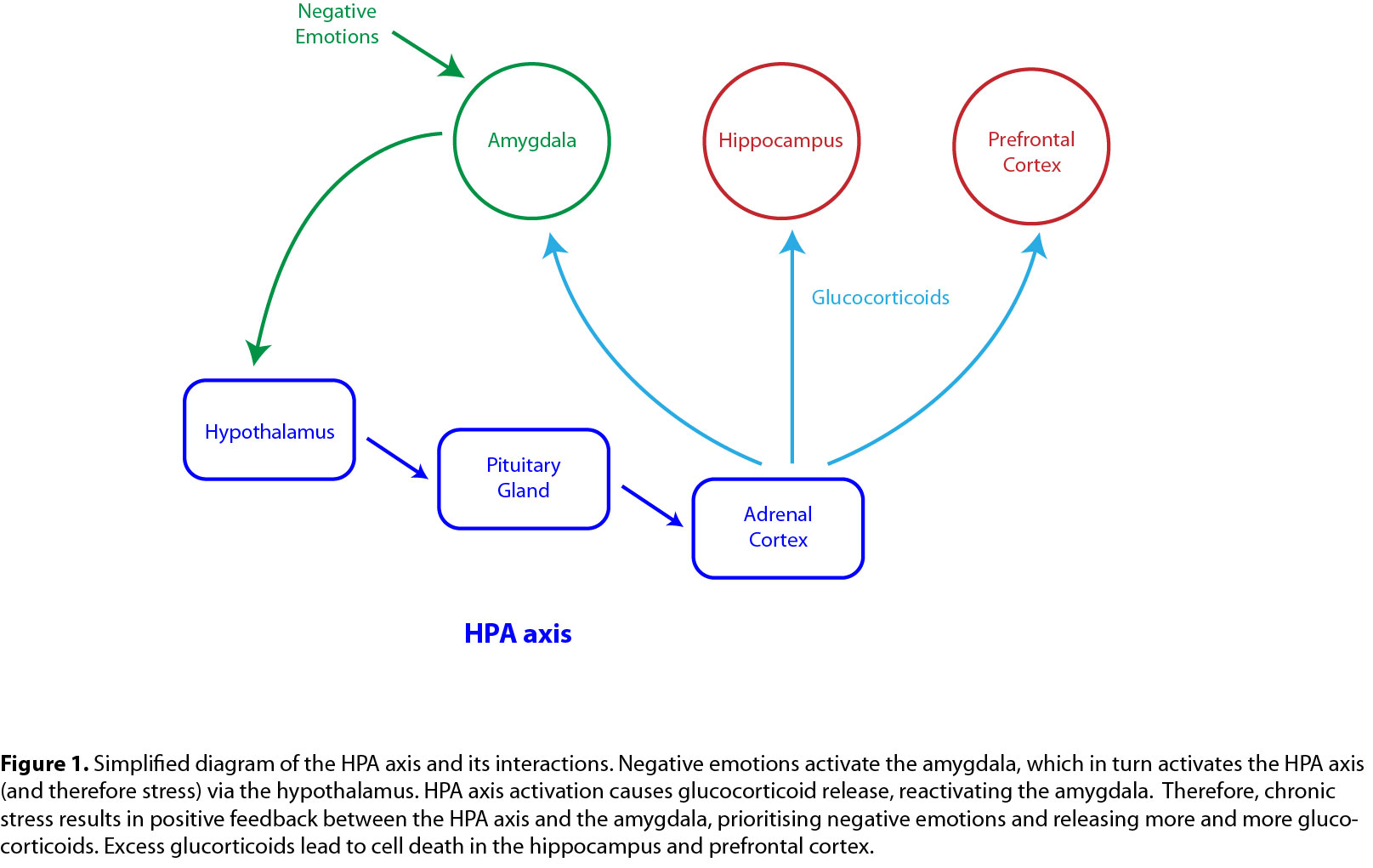
The stress response itself occurs primarily within the so-called HPA axis, involving the hypothalamus, pituitary gland, and adrenal cortex (Figure 1). Ultimately, the adrenal cortex releases glucocorticoids, which have effects throughout the body on metabolism and immune function, amongst other things. Glucocorticoids also inhibit earlier steps of the stress response within the hypothalamus and pituitary gland, preventing the system from becoming overactive.
But what triggers the stress response in the first place? The major activating input comes from the amygdala, a part of the brain important for the processing of emotions, particularly negative emotions. Thus when someone experiences negative emotions, the amygdala becomes more active, which can trigger the stress response in the HPA axis. The released glucocorticoids then trigger a positive feedback loop with the amygdala and negative feedback loops with the hippocampus and prefrontal cortex (Figure 1). If the balance of excitation from the amygdala and inhibition from the hippocampus and prefrontal cortex favours HPA activation (amygdala excitation > hippocampus, prefrontal cortex inhibition), positive feedback occurs and chronic stress and depression can result. Chronic stress produces excess levels of glucocorticoids, which can lead to the death of neurons, particularly in the hippocampus. This may be relevant to the mode of action of the most commonly prescribed antidepressant drugs, SSRIs (selective serotonin reuptake inhibitors; see below).
How do brain networks produce major depression?
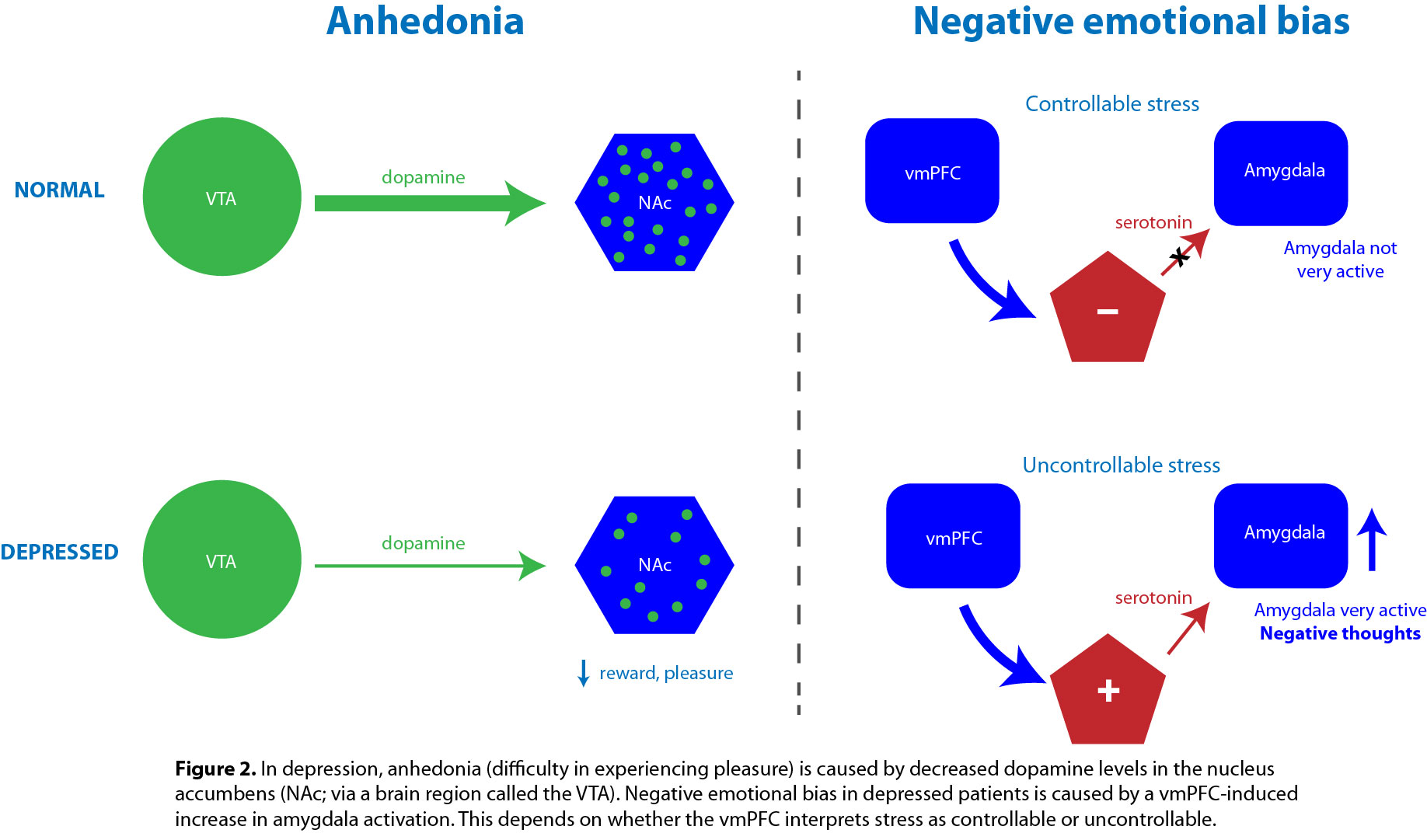
Psychologically, hallmarks of major depression include the overemphasis placed on negative events and emotions (negative bias), and the state of anhedonia (difficulty in experiencing pleasure). Together, these factors conspire to make the depressed subject feel as though everything is terrible and that nothing is really worth doing. Two important brain regions for this are the amygdala, for negative emotions, and the nucleus accumbens, for pleasure (see Figure 2).
Negative emotional bias
A lot of evidence indicates that the amygdala is particularly active when a human or animal experiences negative emotions (in animals, this is often fear). With regard to depression, neuroimaging studies in humans show that in response to viewing sad faces, the amygdala of depressed people is extremely active when compared to the amygdala of non-depressed people, yet when viewing happy faces, amygdala activity is not distinguishable between the two groups. So an overactive amygdala may be one contributor to depression.
But what is it about the depressed brain that causes the amygdala to be overactive in the first place? A plausible idea is that an out-of-whack stress response is to blame. Stress alone doesn’t necessarily lead to depression, however – instead it’s the ability to cope with stress that matters. The question, therefore, is whether the stress is controllable or not. The ‘answer’ to this question seems to be decided within the ventromedial prefrontal cortex (vmPFC). The vmPFC can affect amygdala activity via a serotonin-releasing intermediary: if the stressor is controllable, the vmPFC ultimately makes the amygdala inactive, but if the stressor seems uncontrollable, amygdala activity increases and triggers a stress response (Figure 2). Thus in the “I can’t handle this stress” brain, the lack of activity in the vmPFC favours amygdala activation and therefore an excessively negative mood. If this sequence is prolonged, excessive glucocorticoids can be released, causing damage both in the hippocampus, which provides a major input to the vmPFC, and in the vmPFC itself. The result of this stress-induced damage is that vmPFC activity decreases, leading to further amygdala activation and a negative emotional bias.
Anhedonia
Pleasure comes from doing things that we find rewarding. In our brains, the feeling of reward can be induced by activating a specific pathway in which the neurotransmitter dopamine is released into the ‘reward centre’ of the brain, the nucleus accumbens (NAc) (Figure 2). Experiments in animals have shown that releasing dopamine into the NAc is enough to drive reward-seeking behaviour, and that stimulating particular neurons within the NAc can do the same.
Anhedonia – the inability to experience pleasure, or the lack of motivation to seek reward – must be caused by some problem with the dopamine reward system and the NAc. In humans, neuroimaging studies have shown that in response to reward, the NAc of depressed subjects is less active than in non-depressed people. In animals, researchers have shown that animals subjected to chronic mild stress (to induce ‘depression’) need a bigger reward to achieve the same task as normal animals. Furthermore, ‘depressed animals’ show changes in the way dopamine is released and processed in the NAc.
Summary
The neurobiology of depression is pretty complicated. The inability to cope with stress plays a major role in developing depression. An overactive amygdala, (mis)regulated by the prefrontal cortex, is a key component of this. In addition, the overactive amygdala likely creates a cognitive bias towards interpreting the world, and self, negatively. Making matters worse, the increase in negative thoughts and emotions seems to occur alongside dysfunction in the brain’s reward system, particularly in the nucleus accumbens (NAc), in which the rewarding effects of dopamine are lessened. These biological findings are consistent with behavioural observations of a negative cognitive bias and anhedonia in people suffering depression.