PTSD in military personnel
This weekend Australia will commemorate the 100th anniversary of the ANZAC landing at Gallipoli in World War I. Anzac Day serves to remind us not only of the sacrifice made by those present at Gallipoli, but of all defence personnel since that time who have served our country. When we think of Australia’s military personnel, we think of the sacrifices they’ve made, their bravery, and perhaps of the stress they and their families go through while they are deployed. We tend not to focus on how soldiers handle the return to civilian life, particularly with regard to their mental health. Yet this is a serious issue that’s predicted to become more pressing in coming decades, with many, many veterans of armed conflicts developing mental health problems due to their military experiences.
Post-traumatic stress disorder (PTSD) is probably the most prominent mental disturbance seen following military deployments, with depression and complications from traumatic brain injury also common. As the name suggests, PTSD results from exposure to single or multiple traumatic events and evokes feelings of fear, horror, and helplessness. PTSD often also leads to clinical depression, severe drug and alcohol abuse, and may increase the risk of suicide (it has been estimated that 22 US veterans kill themselves every day). These consequences can be devastating for friends and family of the affected. Symptoms fall into 3 clusters, including re-experiencing the traumatic event (flashbacks, nightmares and intrusive thoughts), avoidance (emotional detachment, avoiding cues, social anxiety) and enhancement of particular physiological responses to triggering stimuli (hypervigilance, enhanced startle, shortness of breath).
It’s important to note that only ~15 per cent of people exposed to trauma develop PTSD, although repeated exposures increase this likelihood. Both early life trauma and genetic factors probably determine the differential susceptibility to PTSD amongst those exposed to the same event(s). To delve into this possibility, the Gallipoli Medical Research Foundation and RSL Queensland recently announced a $5 million initiative directed, in part, at identifying genes that are predictive of susceptibility to PTSD.
The statistics for PTSD amongst defence force personnel make sobering reading. Although the Australian Army states on its website that less than 2 per cent of its personnel develop PTSD following operational deployments, the figure is contentious. A US study found that while 9% of Iraq and Afghanistan war veterans had PTSD shortly after returning from deployment, that number had increased to 31 per cent just one year following deployment. Clearly, lifetime incidence will be even higher than this, meaning that rates of PTSD in military personnel greatly exceed that observed in the general population (3–5 per cent lifetime risk).
Current Treatments for PTSD
Treatments for PTSD can be pharmacological (i.e. with drugs) or non-pharmacological. Pharmacological approaches typically use the same type of drugs used for treating depression, namely SSRIs (selective serotonin reuptake inhibitors). For PTSD, the benefits of SSRIs are debatable. Although some studies have found complete remission in 20-30 per cent of patients, many others have found no difference between treatment with SSRIs and placebos. Another class of drug used for PTSD management is the benzodiazepines, which increase inhibitory neurotransmission. Benzodiazepines are also only occasionally effective, and they possess sedative and addictive properties as well as the potential for abuse. Overall, currently available pharmacological treatments of PTSD are therefore largely inadequate, although they may be suitable for some patients.
A more effective alternative to pharmacological PTSD treatment, particularly when intervention occurs early, is the use of psychological therapies. One approach that has proven effective for reducing PTSD symptoms is cognitive behavioural therapy (CBT). The aim of cognitive behavioural therapy is to realign the way that the patient interprets the world around them. In exposure therapy, which is a form of CBT, the goal for PTSD treatment is to lessen the patient’s negative reactions to the traumatic stimulus, which involves repeatedly presenting the stimulus in a safe environment. The patient then becomes desensitised, learning that the stimulus is in fact harmless and does not portend any danger. The underlying neurobiology of exposure therapy is studied extensively in animal models using a paradigm known as fear conditioning.
The Neurobiology of PTSD – Fear Conditioning and Extinction
In PTSD, traumatic memories are inappropriately triggered by non-threatening stimuli. This situation is mimicked in a widely used animal model of memory termed ‘fear conditioning’, which is crucially dependent on a part of the brain called the amygdala. In this associative form of learning, presentation of an aversive stimulus (for example, a small electric shock to the foot) coincides with an innocuous stimulus (for example, an auditory tone). After a small number of such pairings, the animal becomes fearful when the tone is presented alone. It’s like Pavlov’s dogs, but with a fear-inducing stimulus instead of food. If the auditory tone continues to be presented without the electric shock, the animal gradually learns that the tone is no longer predictive of anything traumatic, and stops exhibiting fearful behaviour. This process of non-reinforced tone presentation is called ‘fear extinction’, and is analogous to the exposure therapy used by psychiatrists to treat PTSD. Studying fear extinction might therefore help us to better treat PTSD – if we can increase fear extinction, maybe we can make PTSD less of a burden.
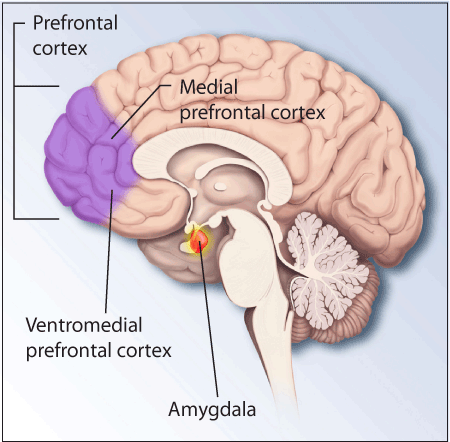
So what do we know about fear extinction? First, the fear conditioning memory (the tone predicts trauma!) is completely separate from the fear extinction memory (the tone is safe!); one can be altered without affecting the other. Second, the critical brain structures involved are the amygdala, hippocampus, and prefrontal cortex, and interfering with particular aspects of this circuitry has successfully decreased fear levels, at least in mice. Third, aspects of the extinction memory are encoded epigenetically, in modifications to gene expression, and preventing or promoting these gene expression changes can alter the strength of the extinction memory (again in mice). Together, this knowledge represents progress in understanding how the associative, emotional aspect of traumatic memories can be modulated, which may be necessary for future treatments of PTSD.
There are, however, things to be aware of when comparing simple fear conditioning and extinction with PTSD. First, the studies into the biological mechanisms of fear memories are conducted in mice, in whom the circuitry and genetic modifications likely differ from those in humans. Second, it’s not clear whether in studying fear conditioning we are studying a ‘normal’ fear response or a response gone awry, such as occurs in PTSD. One important characteristic of the maladaptive fear memories in PTSD is generalisation – reacting not only to the actual cue with fear, but also to non-identical cues. For example, to a subject with PTSD, a lawnmower might sound sufficiently similar to a helicopter’s rotors to make them think they are back on the battlefield. Fear conditioning in rodents has revealed that only some animals generalise their fear, whereas others do not. Further research will hopefully give clues as to what is responsible for these differing responses. Third, in humans, genetic factors and early life traumas can increase susceptibility to PTSD, yet these factors have not been investigated deeply in fear conditioning research.
To understand the biological roots of PTSD, one of the most important aspects is probably to investigate what makes a normal fear response transition to a PTSD-like, maladaptive, generalised response. If we can figure this out, we may be able to prevent or reverse the transition. At the very least, it should increase the likelihood of developing effective pharmacological or other therapies.
Recommended reading
Article from the Weekend Australian magazine (2013)
Professor Pankaj Sah – Neuronal circuitry underlying fear conditioning and fear extinction
Associate Professor Tim Bredy – Epigenetics of fear conditioning
Professor Bryan Mowry – Genetic and imaging-based indicators of PTSD



